A testicular biopsy is a diagnostic procedure where a small segment of testicular tissue is removed for laboratory assessment. This is a crucial step in a comprehensive infertility treatment plan, especially when a semen analysis suggests the presence of abnormal sperm or when other non-invasive tests have failed to determine the cause of conception difficulties. In some cases, it may also be performed to evaluate a lump discovered during a testicular self-examination.
THE TESTICULAR BIOPSY PROCEDURE
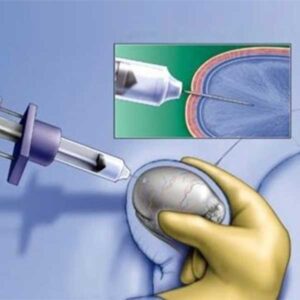
Depending on your specific needs and the doctor's recommendation, the biopsy can be performed in two primary ways:
1. Open Testicular Biopsy
An open biopsy is often performed in a clinical setting or surgical center. After the area is cleaned with an antiseptic solution, a local sedative is administered to ensure the patient is comfortable and the area is numb. A small incision is made in the skin of the scrotum, and a tiny piece of tissue is removed. The incision is then closed with fine sutures. If required, the procedure is repeated for the other testicle.
2. Percutaneous Needle Biopsy
A needle biopsy is a less invasive testicular biopsy technique. Using a specialized needle, a tissue sample is obtained without the need for a surgical incision. Patients typically only feel a slight pressure or a pinprick sensation. While efficient, a needle biopsy may not be recommended for all patients depending on the underlying diagnostic requirements.
PRE-BIOPSY CARE & INSTRUCTIONS
Medication Guidelines
To ensure a safe procedure, patients should avoid taking anti-inflammatory medications or drugs containing ibuprofen for at least one week prior to the biopsy. Always consult with your specialist at Myra IVF before stopping any prescribed medications.
Pediatric Considerations
While rare, a biopsy may be necessary for younger patients. This is typically only performed on individuals older than 12, with careful preparation based on the child's age and medical history.
WHY IS A TESTICULAR BIOPSY RECOMMENDED?
The primary indication for this test is to identify the root cause of male factor infertility. When a semen analysis shows low sperm count or abnormal morphology, a testicular biopsy helps our specialists determine if the issue is with sperm production or a physical blockage.
Furthermore, if an ultrasound suggests a suspicious lump, the biopsy serves as a vital tool to determine if the growth is benign or requires further oncological intervention.
UNDERSTANDING YOUR RESULTS
The results of your testicular biopsy are integral to your infertility treatment journey. Abnormal results may indicate hormonal imbalances or production issues within the testes.
If the biopsy shows that sperm development is normal but the semen analysis remains poor, it often indicates an obstructive issue (a blockage in the tubes). These blockages can frequently be corrected through specialized surgery, paving the way for successful conception.
POTENTIAL RISKS AND RECOVERY
While generally safe, there is a slight risk of minor bleeding or infection. You may experience mild soreness or swelling in the scrotal area for 2 to 3 days following the procedure. These symptoms are normal and typically resolve quickly with rest.
Frequently Asked Questions
When is a testicular biopsy recommended?
A testicular biopsy is recommended when semen analysis shows no sperm (azoospermia) to determine whether sperm production is occurring in the testes. It helps distinguish between obstructive azoospermia, where sperm are produced but blocked, and non-obstructive azoospermia, where sperm production itself is impaired. The results guide further treatment decisions.
Is a testicular biopsy painful?
Testicular biopsy is performed under local or general anesthesia, so the procedure itself is painless. Most patients experience mild discomfort and swelling for a few days afterward. Recovery is typically quick, with most men returning to normal activities within one to two days. Pain medication is provided for post-procedure comfort.
Can sperm from a testicular biopsy be used for IVF?
Yes, sperm retrieved during a testicular biopsy can be used immediately for ICSI (Intracytoplasmic Sperm Injection) as part of an IVF cycle. If not used immediately, retrieved sperm can be frozen and stored for future IVF cycles. This gives men with azoospermia the opportunity to father biological children through assisted reproduction.
